The healthcare industry completely relies on DME medical billing for financial stability and to provide high-quality patient care. DME is a collection of devices and equipment that healthcare professionals prescribe to patients in their recovery or to manage chronic conditions. It is important for healthcare professionals to understand the complexity of DME billing in order to get timely payment and stay financially stable in the long term.
However, DME billing is becoming more challenging due to changing regulatory policies and payer-specific rules. Additionally, documentation, coding, and claim submission errors can
result in denials, delayed payments, and compliance issues.
In this blog, we will understand DME medical billing and the best practices to improve it.
Let’s begin with an understanding of DME billing.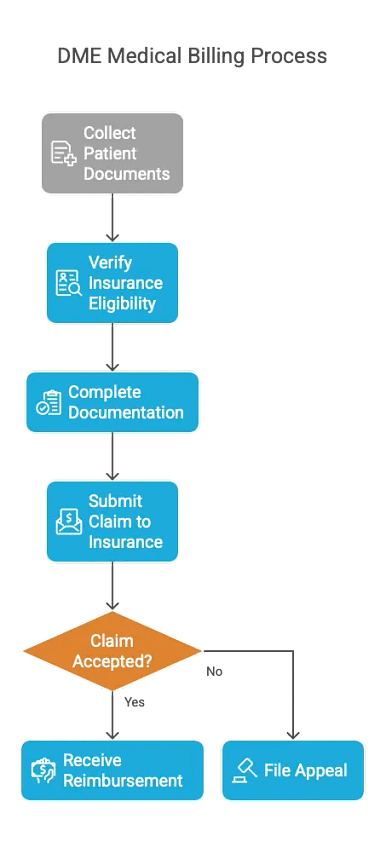
DME medical billing is the process of submitting and managing payment claims for durable medical equipment, prosthetics, orthotics, and supplies. DME comprises several medical devices and equipment created for daily use of patient which include wheelchairs, oxygen, crutches, nebulisers, and prostheses.
DME billing calls for several procedures to obtain suitable compensation. The initial stage is getting various patient documents—such as demographics, coverage, and medication data—from healthcare professionals. This information is required for a complete and accurate durable medical equipment reimbursement. The next step is to confirm DME item insurance eligibility and coverage after gathering patient data. This requires knowing any approval limits and checking that the patient’s insurance covers that specific device.
After eligibility has been verified, the DME provider has to fulfill insurance company and healthcare regulatory documentation and paperwork requirements. A licensed healthcare provider must prescribe the equipment, document its medical need, and keep complete records of the patient’s condition and history. Following documentation, the DME provider sends a claim to the insurance company for reimbursement. The claim includes the patient’s diagnosis, prescribed equipment, service dates, and DME cost. Once the insurance company gets the claim, they look at medical necessity, insurance coverage, and billing laws to decide whether to accept or reject the claim. If the claim is turned down, the DME provider may need to file an appeal with more information or proof
This is the initial phase in DME medical billing. According to the regulating authority, durable medical equipment has to meet a certain medical function and has to be used for at least three months. This indicates that the equipment benefits people with particular health concerns or conditions. Thorough documentation of the need for medical services, including patient medical records, physician progress notes, and the patient’s care plan, will help to avoid claim denials.
A physician’s prescription is necessary for reimbursement of medical equipment. The prescription must specify the necessary equipment, the reason for its use, and the intended application for addressing the patient’s condition. It is crucial to make sure the prescription is accurate and matches the DME medical billing equipment request. Practices should perform regular audits of prescriptions to verify that all essential components for insurance and Medicare DME billing compliance are present.
Numerous insurance providers, such as Medicare, mandate prior approval before the submission of DME claims. Prior authorisation requires consent from the insurer. This process confirms that the equipment is included in the patient’s insurance coverage. Failing to follow this process can result in claim denials.
Accurate record-keeping is necessary to make sure that DME payment follows the rules. Carefully writing down the patient’s medical history, doctor’s orders, clinical notes, and proof of delivery is very important. This thorough record-keeping makes sure that submissions follow the rules set by payers and reduces the chances of mistakes that could lead to audits, claim rejections, or fees. These records can include information about the patient’s health, their finances, and detailed notes from the doctor that explain why the device is needed.
Coding is essential to assign the correct HCPCS codes to each piece of equipment, as these codes pertain to durable medical equipment. Accurate coding ensures the correct submission of claims and the appropriate categorisation of equipment based on medical necessity. It is crucial for providers to apply the appropriate modifiers to denote unit dose forms or particular conditions related to the equipment. Inaccurate coding may result in the rejection of claims.
Another essential element of DME medical billing is proof that shows that equipment was provided to the patient. Evidence of delivery can be anything like signed receipts or electronic tracking systems. Medicare DME billing and private insurers necessitate this evidence of delivery verification to confirm that the equipment was actually supplied to the patient prior to claim approval. Inadequacies in this documentation may lead to postponed payments or reviews.
The billing process for durable medical equipment involves various challenges, such as evolving payer regulations, compliance issues, and the potential for audits. Each insurance provider or governmental initiative has its distinct guidelines, and healthcare providers have to stick to these regulations. Not following these rules can lead to payment delays, denials, and even fraud accusations. This could happen because of things like upcoding, billing for equipment that wasn’t needed, or charging for services that weren’t given.
DME Billing refers to the process of submitting and handling claims for durable equipment that is provided to the patient for a specific purpose.
To get maximum reimbursement in DME billing, ensure accurate coding, documentation, and the prior authorization process, and consider outsourcing experts for billing.
Yes, proof of delivery is essential for DME billing to demonstrate that the equipment was provided to the patient.
Connect with EZ Settle Solutions at 346-335-4093 / info@ezsettlesolutions.com or book a free demo for any assistance or query.
EZ Settle Solutions ensures that claims are sent in correctly, reduces rejections, speeds up reimbursements, and follows all billing rules with 24/7 support.
Durable Medical Equipment (DME) billing requires accuracy, compliance, and proactive management to ensure proper reimbursement and avoid revenue loss. By following best practices such as verifying patient eligibility, using correct HCPCS codes, ensuring documentation accuracy, and leveraging expert billing services, healthcare providers can optimize their revenue cycle.
At EZ Settle Solution, we help healthcare providers in the USA and UK streamline their DME billing process, minimize claim denials, and maximize reimbursements. Contact us today to learn how we can support your billing needs.